CerviGuard is SmartClover's flagship workflow product for cervical-screening teams. The product direction is practical: provide clinicians with a secure workspace where AI can support case triage and workflow management, while medical teams remain in final control of decisions.
- Live product workspace: cerviguard.link
- Public implementation repository: SmartCloverAI/CerviGuard
- Published models and assets: huggingface.co/smartclover
Operational model
CerviGuard establishes a clinical operating model where structured cervical case-material intake, AI-assisted image-signal review, and role-based follow-up are connected in one reviewable workflow. Instead of fragmented files and ad-hoc communication, teams can use one traceable path from intake to follow-up planning.
The objective is not to replace clinical judgment. The objective is to make follow-up signals easier to review, keep triage support consistent, and keep context visible for clinician decisions.
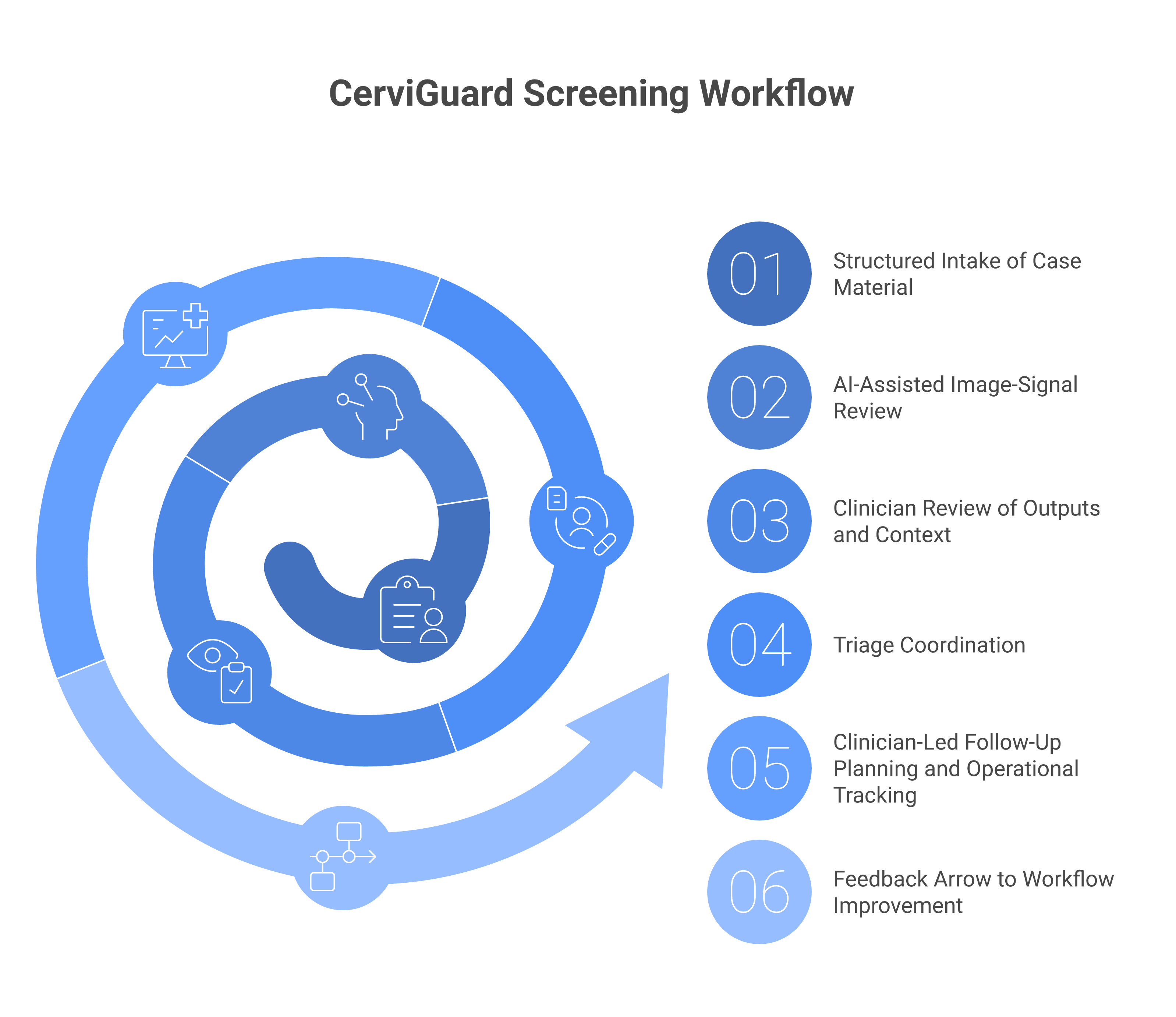 CerviGuard connects intake, review, triage coordination, and follow-up planning in a clinician-led workflow.
CerviGuard connects intake, review, triage coordination, and follow-up planning in a clinician-led workflow.
Why this is tied to field screening and follow-up research
This project draws on Romanian field screening and follow-up research in underserved communities, where teams documented practical barriers to participation and continuity of care. Those barriers include access gaps, trust issues, communication friction, and delayed care pathways.
The same problem patterns are documented in peer-reviewed studies that inform the product direction:
- PubMed 28460211 Qualitative research on Roma women's participation in cervical cancer screening in Romania (Social Science & Medicine, 2017).
- PubMed 35197342 BMJ Open protocol on facilitators and barriers to follow-up after abnormal cervical screening in remote Romanian communities (2022).
These studies help define where a digital clinical workflow can be most useful: continuity of follow-up, transparent review steps, and stronger coordination between clinical and operational actors.
Current direction
CerviGuard is being developed as a clinical workflow product where technology supports teams that already carry responsibility for patient pathways. The objective is to turn field-informed screening and follow-up lessons into daily operational capability, not just research output.
For current product detail and public evidence context, review CerviGuard, Proof, and the Security baseline.
Last reviewed: 2026-05-11.